Modern Midwifery
Designing Equitable Birthing Care
An Interview with Tiffany Townsend, Certified Professional Midwife, Doula, and Certified Lactation Counselor
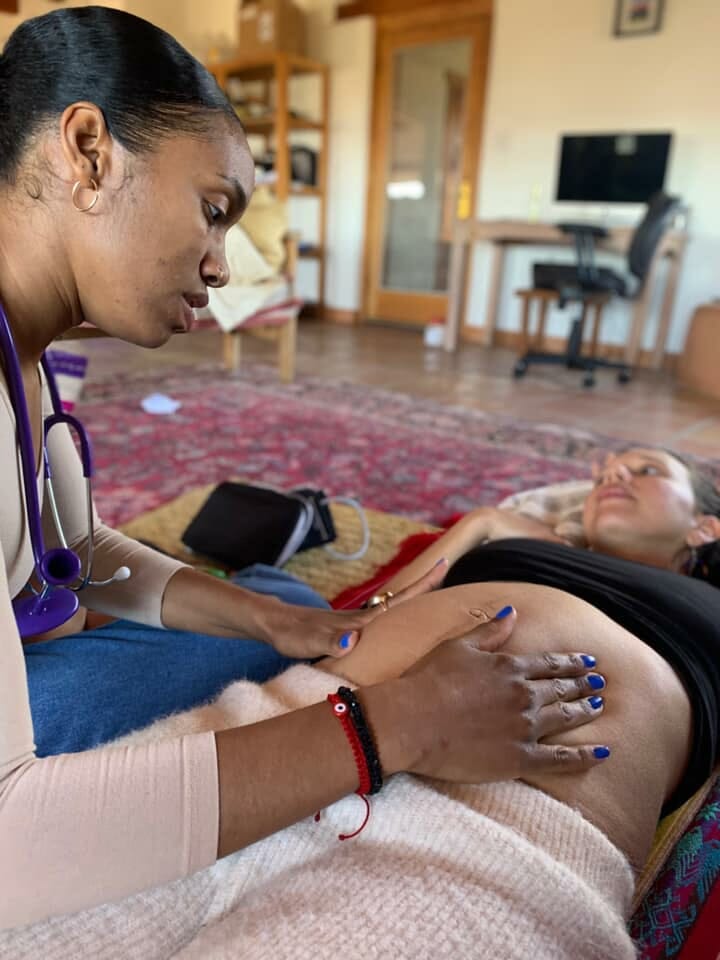
Image courtesy of Tiffany Townsend
Interviewed by Sara Magalio
Tiffany Townsend is a Certified Professional Midwife (CPM) committed to educating families about their options for childbirth and providing nurturing care well beyond American healthcare norms.
She has served her community as a birth worker, support group facilitator, and lactation counselor for over five years. Having attended over 300 births in many capacities, she feels it is important to be able to offer a more holistic approach to care. In her practice, Tiffany also highlights that pregnancy and birth cannot be facilitated with a one-size-fits-all approach, and that everyone should be cared for according to their individual needs.
As the first Black CPM in the city of Grand Rapids, Tiffany has completed numerous certification and training programs that allow her to approach each birth with awareness and respect for various cultures and belief systems. This includes learning under traditional Mexican parteras (midwives) and studying at the Midwives College of Utah. Tiffany has also successfully completed the Neonatal Resuscitation Program (NRP). Tiffany has five children of her own, and has experienced firsthand the benefits and pitfalls of both hospital and home birth, but the thorough, hands-on, and personalized treatment that she herself experienced delivering her last child at home inspired her to continue pursuing midwifery.
It is vital that our clients feel safe, heard, and well cared for in order to establish a safe space for discussing all aspects of care. — Tiffany Townsend
Sara Magalio: I read that your grandmother was an OBGYN and that you have been interested in the field of care surrounding birth from an early age. What inspired you to go into the field of midwifery?
Tiffany Townsend: I am a first-generation American on my maternal side, my family is from the Dominican Republic, and my grandmother was an OBGYN, who was not a fan of traditional birth. I was always called to birth work, because I got to see my grandmother work with Haitian immigrants in the Dominican Republic. I would spend most of my summers in the DR during my childhood. As a young person, I remember watching my grandmother take care of those who were usually overlooked, and that’s how I realized that I wanted to go into a profession in birth care.
I also got pregnant very young, I was 16 when I had my first child, and the treatment that I received in the hospital for that first birth was just really bad. I was not educated. I learned everything about my pregnancy on my own at the library. I initially thought that maybe they were treating me like this because I was 16, and because I was so young there was this expectation that I could never be a good mom. Then I had two more children while married, and the treatment was the same.
I found over time that hospital birthing was not a professional fit for me, because the lack of compassion and bedside manner was something that I never wanted to participate in. Also, just knowing the history of obstetrics and gynecology, I just did not see where I could fit in, in a system that has not seen true reform or change since its inception.
Then I had a home birth with my last daughter, and I was amazed by the compassionate care I received, and the ability I had to retain my autonomy and make my own informed choices throughout the experience. It was the first time that I received truly competent care, and I have five children.
I used to think that the scariest thing about having a baby was the action of giving birth, but I came to find that surrendering to a system that was never really created to protect me was what I really feared.
When I had my home birth with my last child, I was already a birth worker, but the experience encouraged me to start schooling to further my career. I have been recently licensed, and I am the first Black woman in Grand Rapids, Michigan to be a certified professional midwife offering out-of-hospital birth in Grand Rapids.
SM: What, if any, were some of the biggest obstacles that you faced breaking into this profession?
TT: I think it’s very important to note that Black midwives make up just 2 percent of the midwifery population. I think that this speaks volumes to how so many systems are broken. My being the first Black CPM is not something that I celebrate with joy or excitement, because I should not be the first. There should be more midwives of various races and backgrounds to provide care for their communities. We see the data that shows that when people, especially people of color, are provided for by people who understand their culture, then they have better outcomes. (1)
I also struggled with purchasing a lot of the materials and equipment that I needed for my schooling. I was very fortunate to start out at the Midwives College of Utah with a full-tuition scholarship, but I still had trouble affording the supplies list, because we were expected to buy equipment like suturing materials and IV supplies. I continued on to finish up my licenseship in El Paso, Texas, where I also had a scholarship, but there was still that struggle of worrying about paying the rent and how I was going to finish my education. A big part of my journey has been acknowledging the hardships I went through to get where I am, and I am also so grateful for my community, who supported me through all of this and helped me to succeed.
SM: For those who are not as familiar with the options available for birthing, can you touch on the differences between a home birth versus one at a hospital?
TT: A general component of hospital birth is that when you go into the hospital, you are often trading your autonomy for provider convenience. I also want to make it clear that I do not think that OBGYNs are terrible people, but I will say that OBGYNs are surgeons, and when surgeons see an issue, the solution is surgery. This is why we see a lot of hospitals with very high rates of cesarean sections. (2)
Especially with COVID-19 influencing medical procedure and protocol, I have had a lot of late transfers into my practice, because doctors are telling mothers that they should just be induced at 37 weeks for the sake of convenience for the hospital. There is nothing objectively wrong with doing this, but then we run into the problem of the cascade of interventions, and the issue of progressive decisions being made for the mother that takes away her autonomy.
Of course, the luxury of having the epidural is a pro of going to the hospital, and in talking about the pros of the epidural, we also have to address the cons, and how having an epidural can increase the need for a c-section. (3)
With a home birth, you are definitely having one-on-one care with your provider. The person that you hire is the person that is most likely going to attend your birth. There is a lot more room for personal attention. My prenatal visits are an hour to an hour and a half long. For my clients who have already had a child but then change from having a hospital birth to working with me, they are often surprised by the length of their visits and the detailed attention that they receive. We go through everything together, from diet, bowel movements, and sleep patterns to stress level and emotional changes, so that I can connect my clients to resources and be proactive if someone is more prone to having a hemorrhage or having postpartum depression. After the baby is born, my clients are also not waiting six weeks to see someone. I’m there 24 hours after the birth, then at five days, 12 days, four weeks, and six weeks. If there are any issues with breastfeeding or depression, et cetera, it can be addressed quickly and effectively, so that no problems slip through the cracks in that six weeks new parents normally wait before they see a provider.
Also, there is the cost and insurance piece to take into account. I really wish that more insurance providers covered home birth. I am doing so much to raise funds to make home birth as accessible as possible. The con to hiring a midwife is that if you can’t pay the $4,000-$7,000 that it can cost, then you can’t have a home birth. I never want to turn anyone away who may not be able to afford a home birth when they want one. In many states, Medicaid does cover home birth, but Michigan is not one of those states, unless you go to a birthing center. Obviously, there are a lot of hurdles to get through to making home birth fully covered, and it’s especially important to get that moving now, because as we’ve seen with COVID-19, there is a skyrocketing rate of women who are not having babies at the hospital anymore.
Midwives are, despite the preconceived notions, trained professionals, and especially with all of the licensing requirements that have been put into place over the years, the level of education is only increasing as the medical field progresses.
SM: What are some of the biggest misconceptions about home births that you have encountered during your career?
TT: A big misconception that I generally get is that midwives do not have adequate training or that we do not have any of the equipment that is provided at the hospital. In reality, I am bringing everything from IV supplies, medicine for hemorrhaging, resuscitation equipment, and oxygen, just in case there is an emergency. Thankfully I have never had an instance where emergency transport was necessary, but of course we know that sometimes complications can happen in a birth that are not anticipated. Midwives are, despite the preconceived notions, trained professionals, and especially with all of the licensing requirements that have been put into place over the years, the level of education is only increasing as the medical field progresses.
Looking at the Black community specifically, midwives have sustained the Black community forever, even before midwives were officially licensed, when the wisdom was passed down through tradition and ancestral teachings. Midwives have even helped assist with the integration of Black families going into the hospital for childbirth, but at the same time the childbirth mortality rate skyrocketed in our community, which is the opposite of what should happen when receiving hospital care. In essence, just assuming that midwives are not trained and are not able to handle emergencies is the biggest misconception that we face.

SM: You have studied with various organizations involved in the birthing process, including Abuelita Parteras (Grandmother Midwives), Maternidad La Luz, MEAC Accredited, Midwives College of Utah, Indigenous Communities of Mexico, and DONA International. What are some of the biggest takeaways that you have from working with these organizations?
TT: Speaking to my connection with the Dominican Republic, in Spanish-speaking communities, there is a lot of overlap in the practices surrounding birth. For instance, the concept of the “Cuarentena” is basically postpartum confinement to your home for 40 days as a mother, where you’re avoiding the elements and allowing your body to heal. We believe that the “aires” or the wind, can contribute to illnesses in the postpartum period and beyond. In America, it is a very different mentality usually, with mothers trying to bounce back as quickly as possible.
I think that what I have learned mainly from studying other cultures’ birthing practices is the importance of continued care postpartum. Usually the pregnancy and actual birth are focused on as the biggest elements, but the way that we care for mothers postpartum is something that is vitally important for the health of both mother and baby in the future. Looking at nutrition, facilitating the mother’s body slowly recovering, and thinking about mother and baby as a unit and not solely focusing on the child are all components that I have picked up in studying different methods and cultures. I also think that it’s extremely important to acknowledge and respect different people’s cultures and desires when facilitating a birth.
Some of these things may be superstitions and not based in fact, others like the importance of keeping the postpartum body warm and supported, have been used for centuries to facilitate healing. I personally remember being in the hospital and telling my doctor that I wanted to do a placenta encapsulation, and his thoughts on that were basically, “That’s disgusting, why would you do that?” And that is essentially just an example of lacking cultural competence. In essence, cultural competence is having the ability to understand, communicate with and effectively interact with people across cultures, including being aware of one’s own world view and biases and developing knowledge and positive attitudes toward cultural differences. (4) As a caregiver, being open-minded to the mother’s culture, or just her wishes in general, for how she wants the birth to go is to me extremely important.

SM: Have any of your processes changed or been informed by the increased obstacles that COVID has placed on healthcare?
TT: Obviously we’ve been going above and beyond as far as sanitization, we were already quite diligent, but are taking extra precautions for peace of mind both for us and the family. There is also not as much hugging or closeness in the prenatal care and postpartum care, but I still try to make the experience as warm as possible. One big obstacle has been getting access to the cleaning supplies that we need, because priority has been going to hospitals and other healthcare workers, and midwives were largely left out of this prioritized group. I fortunately had enough stocked to make it through until the shortages improved, but it was a real concern that I wouldn’t be able to do my work, because I would not have the necessary sanitization resources.
SM: Delving deeper into systemic inequalities in birthing care, racial inequity in the quality of care that a woman can receive when giving birth is a significant concern. What are some of the ways that the field of midwifery can help address these systematic problems?
TT: I think it’s very important to stress that the solution to the Black morbidity and mortality rate in childbirth is having competent providers. And how do we accomplish this? By funding Black midwives, helping them to get through school and acquire their supplies, and helping them to be able to go back and serve those in their communities who may not be able to pay for their services. Sometimes our allies will try to come in and help our communities with their own answers, but will not listen to our solutions. It would be the most helpful to just help us with our own ideas and the information we have from actually being members of the community who have experienced the issues firsthand.
If the same hospital system that was practicing gynecology and obstetrics on Black bodies without anesthesia is the same place that we are going to today without any significant reform, then automatically we are going to know that there are biases in that place. I think it is also important to clarify that everyone in the medical field does not have malicious intentions, but that does not mean that they are not inadvertently causing some form of harm. Some of the most racist things that I have seen happen in a medical context have come from amazing doctors who call themselves allies, but sometimes they are just not aware of inherent biases and the need to correct past practices that were considered acceptable. For instance, recently a news article polled residents and compiled data that suggested that Black people have thicker skin and do not feel pain the same way is something that was circulating in the not-too-distant past. (5)
Advocating for more Black midwives is not the only answer; however, reform has to happen in the hospital setting as well. Everyone cannot have a home birth for various reasons, and hospitals should be a safe place for people to go and have their babies if that is what they want and need. Until that is the case, we need more midwives of color, we need more midwives that are culturally competent, and we need people to support the causes that we are advocating for in our communities to level out these morbidity and mortality rates. It should never be the case that women are giving birth unassisted because they are not able to pay for a midwife and are too scared to go into a hospital to receive care, and this is a very real decision that women in our community have to face.
A lot of people are saying that in our community, the ultimate solution to inequalities in hospital births is to make home birthing more accessible, but in reality, everyone cannot have a home birth, so the hospitals must find ways to have culturally competent providers that can change the practices that discriminate against certain demographics of people.
SM: What is one piece of advice you would give to expectant mothers who are unsure of where and how they want to give birth?
TT: My advice is to always trust your intuition, if something doesn’t feel right in the type of care you are receiving. Also, it is crucial to be as informed as possible on the different options available as an expectant mother. True informed consent requires understanding all of the pros and cons of every decision that you make for yourself and your baby. It is not just signing a paper that is presented to you and accepting that because the professional says that everything is going to be fine that it definitely will be, because unexpected complications can always arise, and no two births are the same. I think that a lot of people have the mentality that the primary person who makes the decisions is the healthcare provider, when it is actually the parents. No one should be having the final say in decisions about the pregnancy and birth except for the family. I think that it is important to empower parents to make their voices heard, because ultimately we as healthcare providers are just passing through their lives, but the health and well-being of the child is something that they as parents will be responsible for, for the rest of their lives.
You can learn more about Tiffany’s work here.
You can support Tiffany’s efforts to provide low-cost or free services to mothers in need here.
(1) academicworks.cuny.edu/gc_etds/423/
(2) ncbi.nlm.nih.gov/pmc/articles/PMC3615450/#S6title
(3) ncbi.nlm.nih.gov/pmc/articles/PMC4718011/#jpe.1058-1243.24.4.209.s02title
(4) makeitourbusiness.ca/blog/what-does-it-mean-be-culturally-competent
(5) aamc.org/news-insights/how-we-fail-black-patients-pain
